Solutions & treatments
Focus on psoriasis and seborrhoeic dermatitis
Redness and scales on the face, body and scalp can be linked to two specific chronic diseases that affect sensitive and reactive skin: seborrhoeic dermatitis and psoriasis.

Solutions & treatments
Redness and scales on the face, body and scalp can be linked to two specific chronic diseases that affect sensitive and reactive skin: seborrhoeic dermatitis and psoriasis.
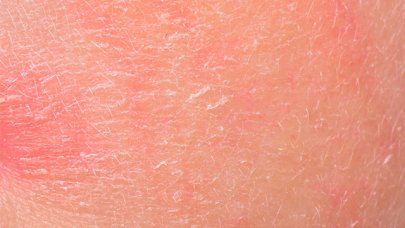
Seborrhoeic dermatitis is an inflammatory scaly condition primarily affecting the face and scalp.
The affected areas of the face are primarily the oily areas (rich in sebaceous glands) on either side of the nose, the nostril folds, the nasolabial folds, the area between the eyebrows and the eyebrows themselves, and the external ear canals. The scalp is the primary area where the disease is found and it triggers inflammatory dandruff that extends beyond the scalp. Other hairy areas may be affected such as the eyelids (causing blepharitis) and the pubis, as well as the beard or chest region in men.

On the scalp, the scales are generally yellowish and oily and do not stick to the scalp. It is possible that they will extend beyond the hairline onto the forehead. For more information, visit the hair and scalp “dandruff and scales” article here.
Seborrhoeic dermatitis progresses in episodes interspersed with periods of total or partial remission. Inflammatory flare-ups may be determined by the seasons and stress. Clinical signs often increase in the winter.
The symptoms vary but there is often itching or a burning sensation.
It is a frequent condition in adults (it affects 3% of the population), especially young adults, but it also commonly affects infants (71% of them), although only temporarily. “Cradle cap” in infants is one sign of seborrhoeic dermatitis.
While some specific conditions promote the sudden onset of seborrhoeic dermatitis, symptoms usually appear in healthy young adults.
Several factors are to blame:

The amount of sebum

Malassezia yeast (fungi) on individuals’ skin (saprophytic flora)
The immune response of the affected person to yeasts that irritate and inflame the skin.
The chronic, recurring nature of seborrhoeic dermatitis which causes redness on the face with or without scales and/or dandruff is a significant source of discomfort for affected people. This discomfort is both social and functional (itching, burning sensations, etc.).
Psoriasis is a chronic, non-contagious skin condition that affects 2 to 3% of the population. It may appear at any age. Specific triggering factors can reveal a genetically predisposed profile and cause lesions to appear.
Psoriasis patches are red (erythematous) and covered with thick whitish scales. They are very clearly defined compared to healthy skin.
The areas most traditionally affected are the elbows and knees (areas that are impacted by microtraumas), but any part of the tegument may be affected. The scalp is one area frequently impacted (particularly the occipital area). When psoriasis reaches the skin folds (groin, armpits, etc.), this is called inverse psoriasis, which is much less scaly. The nails are sometimes affected as well in various ways (thickening, pitting, deformations). Sometimes psoriasis appears on the skin as very small “drop-like” patches or pustules with erythema (redness).
Itching or even burning sensations may be felt in the skin folds. Psoriasis can have a major impact on quality of life, especially if it is widespread or found on particularly embarrassing or hidden areas.
It affects the skin but can also cause rheumatic problems. It affects around 25% of people with a skin condition. This psoriatic rheumatism can be axial (spine) or peripheral (particularly the phalangeal joints).
Psoriasis affects men and women of all ages. However, it begins before the age of 20 in one third of cases and frequently appears between the ages of 20 and 40.
The family is affected in 30 to 40% of cases. Transmission involves several genes (multi-gene) and is not systematic.
Locally on the skin, accelerated epidermal renewal causes patches to appear. With this predisposed susceptibility, certain triggering factors are clear

Climate changes
cold periods in particular

Infectious factors
rhinopharyngeal in particular

Psychological stress
the skin is under the influence of neuromediators and it is “too reactive” here

Local traumas
burns, rubbing and more pragmatically, scratching

Certain medicines
synthetic antimalarials, certain medicines for hypertension, lithium salts, some specific eye drops, etc.

Doctors are familiar with these medicines and there is no need to stop a beneficial treatment if its responsibility has not been proven.
Certain diseases and toxic habits, while not systematic, are often found in psoriasis patients: metabolic syndrome (several signs including being overweight, hyperlipidaemia, hyperglycaemia and high blood pressure), excessive alcohol consumption and smoking. .
If you have redness and scales, visit your dermatologist so he/she can confirm the diagnosis and indicate whether you suffer from seborrhoeic dermatitis, psoriasis or another condition.

In some cases, the doctor will look for what caused seborrhoeic dermatitis to appear. In the vast majority of cases, the doctor will prescribe appropriate treatments, usually anti-fungal treatments. People with seborrhoeic dermatitis should use non-irritating products, understand its chronic and recurring nature, and therefore accept the need for maintenance treatment.
The anti-fungal treatments used are shampoos or creams for the face. In some cases, lithium in gel form is also used. You should avoid using products containing cortisone on the face, as these provide rapid relief but increase the skin’s sensitivity and have a very negative medium-term effect.

The doctor will first assess the scope of the psoriasis, its repercussions, and whether or not there is a metabolic syndrome or excessive consumption of alcohol or tobacco. He or she verifies whether there is rheumatism and if a triggering factor or facilitator can be found.
It is critical to stop scratching since it promotes patches. Stopping toxic factors (alcohol, tobacco) is more than desirable.
Few cases of psoriasis resist therapy, since there are a wide variety of treatments tailored to the various forms. But fortunately, most cases of psoriasis are mild to moderate in scope and do not require any “heavy” treatment. In that sense, local treatments are usually sufficient but need to be applied regularly for this chronic condition. If treatment is discontinued, the lesions reappear.
Local treatments include corticoids and vitamin D derivatives. Moisturise the skin daily with creams to limit recurrences; cutaneous dryness facilitates recurrences. On the scalp, scales can be improved with a keratolytic treatment (salicylic acid, urea).
The general treatments used include phototherapy by a dermatologist, retinoids, methotrexate, ciclosporin and biotechnology medicines.

It’s important to remember that seborrhoeic dermatitis and psoriasis are not contagious diseases. The first line of prevention is to limit factors that trigger or facilitate the condition, such as scratching, which leads to scales, and irritating or unsuitable products.
For psoriasis, you should also avoid temperature variations and cold.
The two diseases are generally improved by sun exposure and sea swimming. While SD and psoriasis are difficult to heal completely, one should not give in to discouragement. Remember that regular treatment will provide prolonged remission and greatly improve your quality of life.

Use a gentle, ultra-high-tolerance soothing cleansing product that is fragrance-free, preservative-free and surfactant-free. Dry your face carefully, without rubbing. Follow this link to learn more about hair and scalp products for treating SD or psoriasis.

Hydration is essential if you have scales. Once or twice a day, gently apply an ultra-high-tolerance treatment that fights inflammatory reactions. It should be fragrance-free, preservative-free and surfactant-free.
You can apply an intense moisturising mask once or twice a week. Once you see an improvement, it’s important to continue the treatments for several months because the inflammation lasts longer, even if it isn’t visible.
If you have psoriasis, you need to control skin dryness caused by winter cold and work harder to maintain effective skin moisture, from your head to your toes.
